Residency
WELCOME!
Please click on the video below to view a message from Dr. Kelly Mitchell, Program
Director
2022 Resident Video
Click below for a more in depth informational video on our residency program from Dr. Kelly Mitchell, Program Director.
Click HERE for Ophthalmology's response to COVID-19
Mission
We welcome this opportunity to introduce the Department of Ophthalmology and Visual Sciences of Texas Tech University Health Sciences Center. The selection of a postgraduate program has a lifelong impact on your career, and we believe that faculty, patient diversity, the basic science and clinical curriculum, and the available facilities are all important factors to consider. We hope this material will better enable you to make this important choice.
Our mission is threefold: to deliver unsurpassed patient care, to pursue excellence in research, and to provide outstanding research and clinical training opportunities for future generations of our colleagues. Our faculty and staff are dedicated to excellence, and through that commitment, we have entered a period of steady growth, represented by new faculty and expanding educational opportunities.
Founded in 1972, our clinic serves a diverse population of patients representing the entire range of ophthalmic pathology -- a key ingredient of any ophthalmology training program. With referrals from all regions of West Texas, Eastern New Mexico, Southern Colorado, and Western Oklahoma, our clinical practice serves more than 25,000 patients annually. Our outpatient clinics are the cornerstone of the teaching program and are operated with emphasis on quality care and the philosophy that all patient encounters are part of the educational experience.
Our basic science research programs have established solid track records in developing well-funded and clinically relevant research. The Ocular Cell Biology Laboratory, opened in 1990, has a significant reputation in cell growth modification, including enhancement and inhibition. Our cellular biologist is working with major ophthalmic pharmaceutical and biotechnology companies, and the electrophysics unit is recognized as one of the finest in the country.
Advantages
Physician Faculty
The vast majority of our clinics are staffed by full-time faculty physicians. Additionally, clinical faculty members in private practice and from the medical school conduct clinics and provide lectures regularly. Residents rotate among the various subspecialty services, and evaluations of residents and faculty members are completed after each rotation.
Research Faculty
The department's basic science program has grown considerably to include highly respected researchers in broad areas of expertise, such as electrophysiology, visual psychophysics, cell growth acceleration and inhibition, and dynamic measurement of accommodation.
Lecture Curriculum
In addition to resident participation at an external basic science Course, full-time and visiting faculty members present a full range of lectures in the basic and clinical sciences.
VA Hospital Experience
We have initiated a local Veterans' Administration rotation and our longstanding Big Spring, Texas, rotation is currently in transition. These rotations provide each resident with experience in treating a large number and wide variety of ocular pathologies. Clinical instruction is provided by full and part-time clinical faculty.
Subspecialty Experience
Residents have the opportunity to work with physicians who are fellowship trained in every major ophthalmic subspecialty. Extensive training and experience in the interpretation of fluorescein angiograms and the diagnosis and treatment of medical retina disorders are integral parts of the program. Residents rotate on the neuro-ophthalmology, low vision, and contact lens services during their first year. Second year rotations include oculoplastics and pediatric ophthalmology, where residents are exposed to a full range of medical and surgical pathology. Extensive experience in surgical and non-surgical management of strabismus is obtained, and the pediatric eye exam and management of amblyopia is emphasized throughout all three years of training. Third year rotations focus on the medical and surgical management of patients with glaucoma, cataract and other anterior segment disorders, and vitreroetinal disorders.
Surgical Experience
Residents participate in a large variety of surgical cases. A surgical laboratory is conveniently located in our facility and is equipped for microsurgery, including phacoemulsification and corneal and vitreoretinal surgery. Graded surgical exposure insures that each resident develops confidence in treating disorders commonly encountered by the general ophthalmologist.
Curriculum
Educational Goals:
To develop the necessary ophthalmology clinical skills for diagnosing and managing basic inpatient and outpatient ophthalmic problems, as well as developing research skills in clinical and/or basic science areas relating to ophthalmology.
Responsibilities:
- Complete the Ophthalmic Pathology rotation.
- Begin work on the American Academy of Ophthalmology‘s Basic and Clinical Science Course.
- Identify subject material for publication
- Make presentations at conferences, including monthly grand rounds.
- Take call on a rotational basis.
- Develop clinical diagnostic skills.
Skills Addressed:
- Refraction techniques
- Slit-lamp examination techniques
- Indirect and direct ophthalmoscopy
- Interpretation of fluorescein angiograms
During the PGY-2 year, residents will work in the department‘s outpatient clinic under the supervision of faculty physicians and senior residents. Responsibilities will increase as clinical skills advance. During this first year, residents are expected to begin clinical or basic research projects, attend conferences and training sessions to promote development of clinical skills, and receive their introduction to surgery.
Educational Goals:
To develop increasing independence in the performance of examinations and procedures.
Responsibilities:
- Continue work on the American Academy of Ophthalmology‘s Basic and Clinical Science Course.
- Serve on rotations at the Veterans Administration facility(s).
- Assist medical students, PGY-2 ophthalmology residents, and residents on electives from other departments.
- Serve as back-up call for PGY-2 residents on a rotational basis.
- Prepare manuscript for publication.
Skills Addressed:
- Surgical skills
- Clinical skills
- Teaching skills
- Leadership skills
During this year, residents will assume greater responsibility in the day-to-day operation of the clinic by maintaining a sustained level of involvement with patients, medical students, primary care residents, and allied health personnel. Also during this year, residents are expected to increase their learning efficiency, as well as research and presentation skills. Surgery participation will also increase.
Educational Goals:
To achieve the clinical and surgical competence necessary for the independent practice of comprehensive ophthalmology.
Responsibilities:
- Complete the American Academy of Ophthalmology‘s Basic and Clinical Science Course.
- Continue to serve on rotations at the Veterans Administration facility(s).
- Achieve a high level of clinical and surgical competence.
- Assume increased leadership role in training medical students, other residents, and technicians.
- Organize and participate in conferences.
- Assist medical students, PGY-2 and PGY-3 ophthalmology residents, and residents on electives from other departments.
- Submit manuscript for publication.
Skills Addressed:
- Surgical skills
- Independent decision making
- Teaching skills
- Investigative and presentation skills
- Leadership skills
Responsibilities during the PGY-4 year will approach those of a full staff physician, and surgical experience will be a major part of the year‘s development. By the end of residency training, physicians should be confident, competent, and highly ethical comprehensive ophthalmologists with a sufficiently strong clinical foundation to enter practice or to proceed with further training in academics for those who have an interest in subspecialty, teaching, or research careers.
Extended Opportunities
Extending service beyond medical education programs are the Great Plains Lions Eye Bank, and the Laser Vision Institute.
The Great Plains Lions Eye Bank is a non-profit corporation supported by the Lions Clubs of District 2-T-2. Its mission is to obtain quality tissue for patients suffering from corneal blindness, to develop educational programs promoting donor awareness, to support health professionals and donor families in the donation process and to promote research for the prevention of blindness.
The Laser Vision Institute offers the opportunity for gaining experience in refractive and excimer laser surgery. Currently, a number of clinical faculty are performing LASIK, PRK, and LASEK at our Laser Center, which owns the latest scanning and active tracking laser - the LADARVision 4000 by Alcon, Autonomous and Summit. We are committed to the concept that excimer laser refractive surgery should be a core portion of the comprehensive ophthalmologist training program. Our senior residents generally performs hands-on PRK and LASIK - often reserved for fellows in many other programs.
Our Basic Science Research laboratories provide research opportunities for postdoctoral fellows, residents, and medical students. In addition, research opportunities are also available for students pursuing graduate degrees in basic or applied sciences at Texas Tech University or Texas Tech University Health Sciences Center. Our electrophysiology and visual psychophysics laboratory offers research opportunities to study patients with rare eye diseases. Those involved in our ocular cell biology laboratory currently investigate factors involved in cell growth, glaucoma, and retinal degeneration. The goals of these programs are to understand the pathophysiological processes involved in various ocular disorders and to develop new therapeutic agents.
FAQs
Questions Often Asked by Resident Applicants and answers by DR. Kelly Mitchell (RPD) and Dr. David McCartney (Chairman)
Over the years, resident applicants have asked many penetrating and perceptive questions. We have collated those questions and added a few we think applicants should be asking as well. While our residency training program has had remarkable stability for many years, the answers given below should be understood to be descriptive of our current status and our plans for the future, although they do not constitute an obligation, or precise prediction.
Q: What are some of the outstanding strengths of your program?
A: Faculty availability/supervision
The availability of our faculty for supervision and the tremendous amount of one-on-one
teaching by faculty members is a unique feature of our program. During surgery, your
faculty mentor will be an experienced, usually subspecialty trained, faculty member,
not simply a more senior resident. We believe this high-quality experience of faculty
staffing, combined with our excellent surgical numbers translates to greatly superior
clinical and surgical training in general comprehensive ophthalmology.
Faculty and resident cohesiveness
We make a conscious effort to choose faculty members and residents who are team players
and who get along well with peers in addition to having outstanding academic and clinical
qualifications. We strive to maintain a collegial, low stress work atmosphere, knowing
that this contributes to promoting an optimal educational environment and outcome.
Residents have mentioned that they feel that department faculty stability is directly
related to the stability and length of tenure of our chair (over 30 years) and residency
program director (20 years). Overall, the average faculty tenure is 15 years at TTUHSC.
Optimal Patient Mix
Another important advantage of our program is our patient mix which is extraordinarily
well-matched to the type of patients and variety of diseases you will see daily the
rest of your career. Many residency programs rely almost exclusively upon clinic populations
who differ substantially in socioeconomic and educational parameters from the populations
those individuals will provide care to following completion of the residency training
program. Such training is less likely to prepare them as well for dealing with a predominately
private patient population. Here at Texas Tech, a remarkably large proportion of our
patient population for whom the residents have primary responsibility will be "private"
by socioeconomic and educational measures, further enhancing your education as a physician.
Q: What is the accreditation status of your program?
A: The Residency Review Committee (RRC) of the Accreditation Counsel on Graduate Medical Education (ACGME) plans to review each program with a major on-site review every ten years. Our last ten-year site visit review was successfully completed in February 2020 and we earned full accreditation. Every year, every program must submit an annual updated report to the ACGME. This report contains information about the major changes occurring in the program and a review of current educational structure and surgical trends and board passage rate trends. Those annual update reports are due to the ACGME in September of each year. The ACGME provided official feedback in January of the next year. In January 2022, our program earned full ACGME accreditation with commendation (for our 2021 update) for having no citations or concerns. Dr. Mitchell has recently submitted our annual update for 2022 and based on our positive trends in surgical numbers he is expecting another strong review from the ACGME.
Q: How well do the residents learn modern phacoemulsification cataract surgery?
A: Extremely well. University Medical Center Hospital and our very soon to open VA Lubbock surgical center and clinic have the top of the line surgical equipment plus microsurgery and phacoemulsification laboratory here at the parent institution with Resident access to this laboratory is 24/7. More importantly, our residents are taught contemporary cataract surgery techniques by experienced faculty cataract surgery educators. The techniques include vertical and horizontal chop, stop and chop, divide and conquer, one-handed, topical anesthesia when appropriate, mostly clear corneal with scleral tunnels as needed.
Q: Does the program use surgical simulation as part of the surgical curriculum?
A: We have 2 simulators available. One EyeSi anterior segment unit is at the Lubbock VA clinic and surgical center and one EyeSi anterior segment with a posterior segment unit that is available 24/7 at the main TTUHSC Lubbock campus. We have observed that such laboratory enhancement has increased the efficiency of our residents in the human operating room, allowing them to increase their case load even further than our already very high numbers.
Q: What is the typical surgical load for graduating residents?
A: Below is the most recent information from the ACGME reviewed data. This shows our overall surgical experience. The table shows the established minimums, the average of our 2022 graduating residents. The blue bar graph shows how our programs compares to the other ACGME residency programs in each of the major surgical areas for the 2022 graduates. Overall, our 2022 graduates finished in the top 89% in overall resident hands on surgical training.
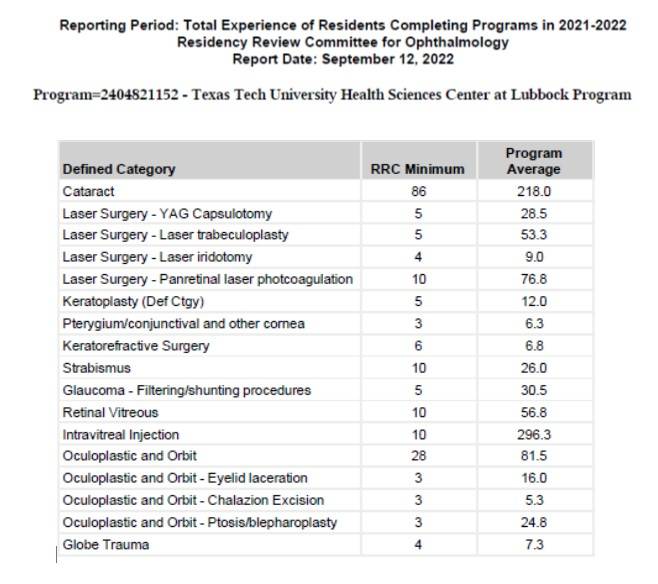
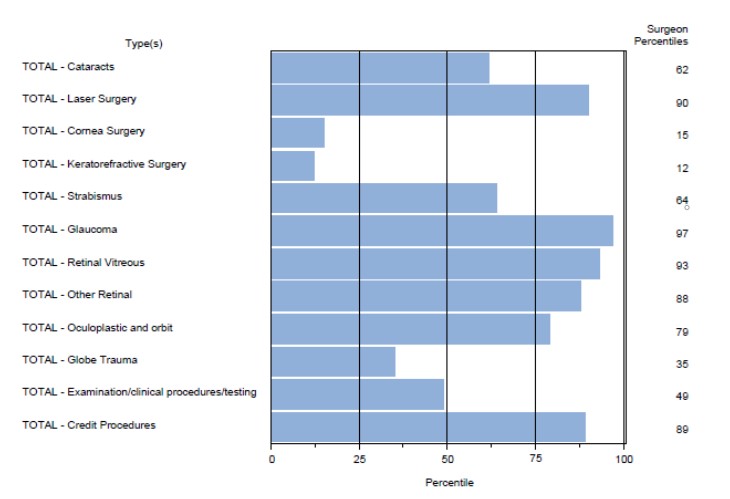
Q: Can you give me an idea of the typical resident rotation schedule and clinical load?
A: Our clinics at Texas Tech are arranged in a modified block schedule around our subspecialty faculty. A typical clinic would be the Cornea / External Disease and Anterior Segment Clinic staffed by Dr. McCartney which generally has two or three residents, and we typically see from 20-30 patients per half day. This generally means that each resident, depending upon level, will see between 4 and 10 patients per half day.
Q: Which rotations do residents complete outside of Lubbock?
A: There are no current rotations outside of Lubbock. A rotation outside of Lubbock that would require a resident to either drive (daily) or have temporary residence there would need to offer an outstanding and uniquely important surgical experience to be considered. Practically, neither Dr. Mitchell nor Dr. McCartney sees the need for such a rotation currently nor is it likely over the next 5 years.
Q: Do you have surgical fellows?
A: Not presently, and there are no plans to add a fellowship program. The faculty of the department remains committed to resident education as our primary educational mission.
Q: Has the program transitioned to include the internship as required by the ACGME?
A. Yes. More specifically, our program choices to use the integrated internal medicine internship model. In this model, our program gets to partner equally with Internal Medicine. The ophthalmology RPD (Dr. Mitchell), helps chose the specific rotations for the ophthalmology interns. He uses feedback from the previous years’ residents to help avoid rotations that are heavy on patient service and light on education. Dr. Mitchell also gets to specify that the ophthalmology interns get to end their IM rotations at the same time (April) and start in ophthalmology all at the same time for a total of 39 months at graduation. Our faculty and residents strongly feel that this helps build early and important camaraderie for our residents.
Q: Are you planning to change program size or number of residents?
A: After a five-year planning process, our program was approved by the Residency Review Committee to increase from three to four entering residents per year in June 2015. We have no plans to expand the program further in the foreseeable future. The current four residents per year size is an optimal balance for resident surgical experience, call responsibility, duties, and our physical facilities.
Q: How do your residents do once they leave your program?
A: The performance of our alumni can be measured in several ways:
Obtaining fellowships
On average, one-third of our residents’ desire and acquire a competitive fellowship.
During the last ten years, we have had fellows train at academic institutions in Boston,
Portland, Omaha, Philadelphia, Morgantown, Montreal, Los Angeles, Dallas, Salt Lake
City, New York City, Atlanta, New Orleans and Albany. Over that last 20 years, 25
residents have applied to fellowship and all 25 have matched.
Confidence of practice
About two-thirds of our graduates do not choose to do a fellowship. I believe this
provides clear evidence of the confidence our alumni feel about practicing general
comprehensive ophthalmology once they have finished their training at Texas Tech.
Furthermore, we have many instances when senior ophthalmologists of groups that have
hired our graduates will call either Dr. Mitchel or Dr. McCartney with compliments
of how well prepared our graduates are to confidently function as new eye surgeons.
Q: When does the interview committee decide upon its rank list and will I have any feedback from the committee regarding my standing after the interview?
A: Our program adheres to the A.U.P.O. and SF Match polices that residency programs will not engage in discussions after the interview with applicants concerning the applicants ranking position. However, if the applicant is concerned that a portion of their application is still incomplete at the conclusion of their interview then they ae encouraged to follow-up with the residency coordinator regarding that specific issue about their application. Simply put, if we interview you then we are very impressed and interested and we would want your application to be complete so we can give you worthy attention during our final ranking process.
Q: Is there a moving allowance or professional development fund?
A. Presently, we provide a $2,000 professional development fund for each incoming resident. The professional development allowance is available to fund professional travel, professional supplies, such as examination lenses and/or loops, and can be used for moving expenses as well.
Q: Where do your alumni tend to practice after they complete the residency?
A: Our residents tend to practice medicine in Texas, the Midwest, Florida and West, with the least number of residents choosing the Northeast for a practice location.
Q: What research opportunities and funding are available to residents?
A: Each faculty member to date has made themselves available as a faculty mentor to assist and guide residents in research projects. Each resident is expected to complete either a case report or a research project. That requirement was appropriately loosened during COVID as usual GME education needed to adapt. Funding is available through the individual faculty research program and/or from other departmental funds.
Q: Do you train residents in refractive surgery?
A: We are committed to providing evidenced based, modern refractive surgery should as part of comprehensive ophthalmologist training. We offer incentives to patients to encourage them to allow resident physicians to perform Class 1 surgical laser surface ablation.
Q: What kind of long-term relationship does your department have with its alumni?
A: The Department sponsors an annual reception for the alumni at the American Academy of Ophthalmology Annual Meeting and, through the vehicle of an annual newsletter and various ad hoc contacts throughout the year, keeps up with the activities of our alumni over time. Naturally, as with all programs, the Department will be responsible for the rest of your career for credentials verification and letters of recommendation and verification to your future employers, hospital affiliates, and insurance plan credentialing offices. In this fashion, the Department very much views our relationship in the long-term perspective. As well, numerous resident and faculty alumni have become philanthropic partners of the Department through their support and gifts to the Department's foundation accounts.
Q: How involved are the faculty with the residents in terms of extracurricular or social activities?
A: The Department strongly supports the need for quality resident family life and healthy recreation to balance the rigors of residency work . Currently, activities in which the residents and faculty commonly participate include departmental holiday/seasonal parties, appropriately vetted industry sponsored events, the annual resident graduation dinner in June. Broadly speaking, the residents typically arrange multiple social activities throughout the year and it would be common place for 1-2 faculty to attend depending on their respective schedules.
Q: Are there any questions you think I should ask in addition to the above?
A: At least one additional question comes to mind. An important measure of the success of a residency training program is the morale of its residents and staff. Although there are occasional personality reasons why an individual resident might be unhappy, it is certainly worthwhile to poll as many residents as possible about their feelings regarding their educational experience. In this regard, we make every attempt to give you maximum contact with as many residents as possible. If you have any additional questions you would like to pose, please feel free to call us. We will make every attempt to put you in contact with as many residents as possible.
Q: What do your residents say about your program?
A: Resident comments emphasizing particular strengths of the program they feel warrant special attention include the following:
- "Thank you to everyone involved in my training and that of future ophthalmology graduates.
The impact of the clinical/surgical/moral lessons learned will stay with me forever.
Matching at TTUHSC was life-changing!"
-
-
- - Dr. Hari - Bodhireddy (Class of 2014) Glaucoma Fellowship, Moran Eye Center, 2015, Private Practice Spokane WA, 2015 to present.
-
-
- Very Strong surgical experience in cataracts, glaucoma, and retina
- All major subspecialties are covered by 1-2 attending faculty.
- Integrated internship now allows a much smoother transition into the R2-4 years.
- The program presently does not routinely schedule educational conferences or other responsibilities (aside from call) on Saturday or Sunday.
- Reasonable call schedule
- Ample vacation is provided by the institution.
- Attractive health, dental, optical insurance for residents and dependents.
- Affordable local housing-many residents actually purchase their home due to the very attractive housing market
Q: How competitive is the Ophthalmology Match Program?
A: The latest match information is available at: http://sfmatch.org/
Q: What qualifications would increase my chances of matching with Texas Tech?
A: Frequently, an applicant asks this question, "What are you looking for in an applicant?" While the program recognizes the obvious reason for asking such a question we are happy to be quite open about our preferences in the qualifications of applicants, as we are really not looking for self-testimony about such qualifications, but rather objective evidence from your established record. Among the qualifications we value most are the following:
- Evidence of a commitment to serving a cause larger than self-interest.
- Positively focused on the needs of others; genuine kindness
- A strong work ethic with the ability to be adaptable; to think on one's feet
- An honest, inquiring mind and effective personal commitment to self-education
- Self-confidence to be able to embrace constructive advice balanced by genuine humility to be able to incorporate coaching into future behavior
- Resilience: the capacity to be challenged and to grow and succeed
- Strong communication skills along with flexibility in interpersonal relationships to become a strong team player
- Demonstration of fair mindedness and evenhandedness in order to be a good and trusted citizen within our residency, department, and the TTUHSC community.
Got Questions?
We're here to help. Contact us if you have questions.
Residency Program Manager
Phone: 806-743-1465
