Rotations
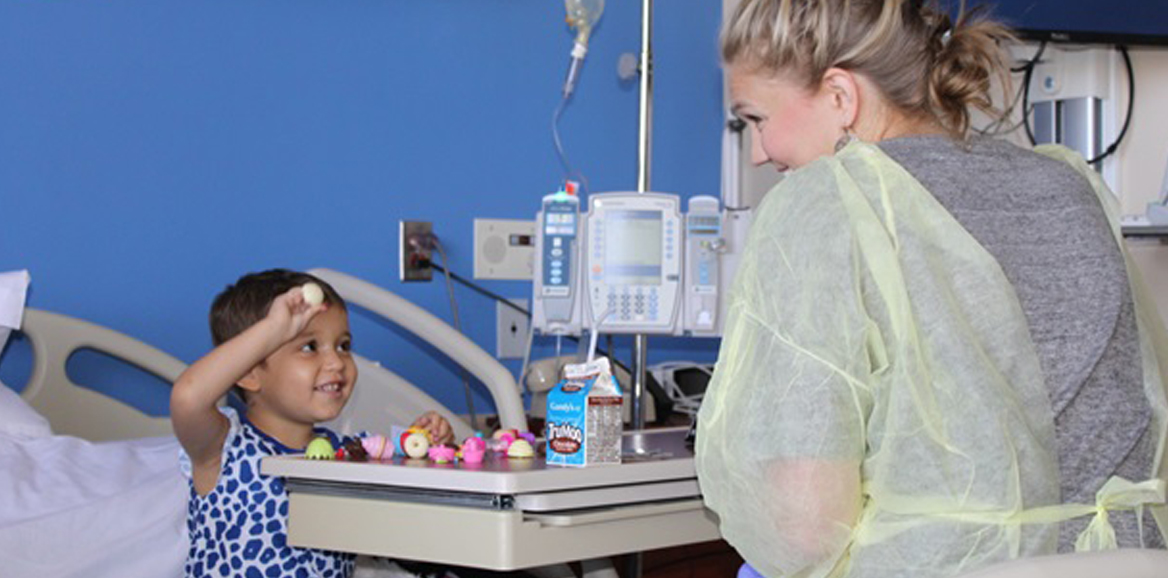
Inpatient Ward
Inpatient ward rotations are located at the Children's Hospital at University Medical Center and Covenant Women's & Children's Hospital. The intern on the ward provides primary care for all inpatients and coordinates care with primary care attending's and consultants. The senior residents provide supervision and teaching while overseeing the care of all patients admitted to the pediatric floor. Attending rounds are held daily. An academic pediatric hospitalist service provides most of the inpatient teaching. Additionally, a PharmD specialized in pediatrics, rounds with the team daily during the week to assist with medication dosing and choices.
Our nursing staff does a superior job of providing patient care that emphasizes the needs of children. They take the time to get to know the patient and the family, to provide education, and to update the parents and patients with details concerning their care throughout the hospital stay. Full-time child life specialists, physical therapists, occupational therapists, speech therapists, and respiratory therapists add to the thorough and comprehensive care.
The 24-hour inpatient resident coverage at UMC is accomplished with the night shift system. The interns are responsible for two blocks of night shift over the course of a year. The intern assists with admissions, covers the inpatient ward and newborn nursery. Senior residents have a night shift block each year. The senior resident assigned to night shift is responsible for all admissions, patient management in the PICU, and supervising the intern. The senior resident answers after-hours nurse-triage calls from parents whose children are seen in the general pediatric clinics. There is faculty supervision for all night shift and on-call residents.
The night shift system allows more flexibility in scheduling and has been a great benefit to our residents. Weekend coverage is provided by residents not on inpatient services- interns in shifts and senior residents on 24hr call. Weekend coverage occurs <1-2 times per month.
A junior or senior resident is assigned to the Pediatric Intensive Care Unit (PICU) at Covenant Children’s Hospital every month and is responsible for admitting and providing care for all PICU patients. The PICU is a 15-bed facility staffed by a 24hr in-house Pediatric Intensivist. The training in the ICU is supplemented by consults on pediatric general surgery patients who come to the PICU for post-operative care or trauma management as well as consults on post-operative care for neurosurgery patients.
During the first and second years, residents are assigned to the newborn nursery at UMC. The resident is responsible for providing patient care as well as parent education and arranging follow-up. The resident also performs all circumcisions (with direct faculty supervision) for newborns on the Texas Tech service whose parents have requested the procedure. The newborn resident also sees patients in newborn follow-up clinic.
The Neonatal Intensive Care Unit (NICU) is housed adjacent to the Family Birthing Center allowing for a prompt transport of a seriously ill infant after delivery. The NICU is a 48-bed unit encompassing care of the most critically ill infants in the Level III nursery and less critical patients requiring intermediate care in the Level II and Special Care Nurseries.
A senior resident is assigned to the NICU every month and is responsible for attending deliveries, admissions, discharges, and providing daily patient care for all NICU patients. The resident also does prenatal consults when requested by the obstetric team. When an intern is assigned to the NICU, they work with a senior resident. Senior residents spend 1 week on nights in the NICU. Senior residents are on service overnight with experienced neonatal nurse practitioners. The residents have an excellent opportunity to further develop procedural skills, including intubations, umbilical lines, and chest tubes. Attending neonatologists supervise the patient care and resident education while rotating in the NICU.
High Risk Clinic
High Risk Clinic is a follow-up clinic for NICU graduates. The clinic is run by a
NICU attending and the infant is followed throughout their first two years. Residents
are invited to spend time in this clinic to gain a better understanding of the care
of the high risk neonate, including management of BPD and identification of developmental
delay.
The ER rotation is done at Covenant Children's ER.
The Pediatric Emergency Room is a Level II Pediatric Trauma Center and staffed with Pediatric Emergency Medicine trained physicians, as well as general pediatricians. Residents will assess and care for patients and conduct procedures such as suturing, splinting, lumbar punctures, etc. This rotation will also provide an opportunity for the practice of other procedural skills such as IV placement and bladder catheterization.
In addition, pediatric residents serve as consultants for the UMC Emergency Room, a Level I Emergency Room. While on pediatric ward, PICU rotation, and on call, residents evaluate patients referred by the emergency room physicians. All patients are discussed with the inpatient pediatric ward or critical care attending prior to admission or discharge home. In addition, consults are received from other services such as the pediatric trauma team.
Our residents rotate through all of the general pediatric clinics run by our Pediatric faculty at the Medical Pavilion, the Medical Office Plaza, and Health Point. Residents have four ambulatory clinic experiences - two during their intern year and one each subsequent year.
The developmental rotation is done in the first year and focuses on differentiating normal and abnormal development as well as recognizing and treating behavioral problems in the pediatric population. Much of the clinical time is spent with a fellowship trained developmental and behavioral pediatrician. Additional time is spent exploring community resources for children with developmental and behavioral problems such as early childhood intervention programs and special education resources. A portion of this rotation is also devoted to abuse and neglect with time spent with Children's Protective Services and other agencies involved in protecting children.
The adolescent medicine rotation at Texas Tech University takes place in three outpatient settings, with the exception of occasional pediatric floor or PICU consultations. Residents see patients in the Adolescent Clinic, which is housed in the Medical Pavilion. They spend one day per week at Hart ISD working at the rural school-based clinic, seeing junior and senior high school students. They also spend a half day each week at the Texas Tech Student Health Sports Medicine Clinic, evaluating sports related injuries.
Community Rotation is a longitudinal experience across all three years of training which incorporates private practice, advocacy, community resources, and public health experiences.
During their Intern year, residents spend time with pediatric dentists and allied health specialists, including audiology, PT/OT, and ECI. They complete medical home training and also look into health disparities locally and nationally. All interns attend the Annual TPS Meeting in the fall sponsored by the Department of Pediatrics.
Senior residents spend a week in the office of a private practitioner of general pediatrics. The goal of this week of community clinic experience is to provide exposure to office management, insurance, billing, coding, and other day-to-day aspects of private practice. Many different practices are available thanks to the excellent relationship that the department of pediatrics shares with the community pediatricians.
Our senior residents also rotate at the Texas Department of State Health Services for a week. Residents learn about communicable diseases, community and environmental health, specialized health and social services, and public health emergency preparedness/epidemiology.
All PGY2 residents annually attend the AAP National Conference & Exhibition. This gives the residents an opportunity to learn about national resources including the most current information related to illness and preventive health care of neonates, infants, children, adolescents, and young adults. Residents are exposed to practice management and health policy issues as well as national child health advocacy campaigns.
All PGY3 residents annually attend TPS Advocacy Day at the State Capitol in Austin, TX where they are provided advocacy training through the TMA and an opportunity to meet with State Senators and Representatives.

Our Pediatric residents develop a truly individualized curriculum based on their career goals. Our program achieves this through our faculty mentorship program. When residents enter our program, they have a career goal and we find that these goals may become refined but often change throughout the intern year as residents rotate through various clinical settings. We encourage the exploration of clinical experiences as they pertain to personal values and professional goals through monthly intern group mentoring. These mentoring session are facilitated by a clinical psychologist who provides supportive counseling and helps the interns process information and manage stress. Career goals are tracked through quarterly meetings with the program director.
In the spring of their intern year, residents are asked to identify a faculty mentor who will serve as an advisor to guide professional development. Then, in conjunction with the program director, residents begin to construct their individualized curriculum blocks. Our program has established tracks for Primary Care (Ambulatory, Inpatient, and Newborn), Critical Care (PICU, NICU, Emergency Medicine), and Subspecialty (various fellowships) with recommended electives and additional subspecialty experiences. These tracks serve as a starting point for each resident and can be further tailored to meet each individual’s professional needs with opportunity to develop innovative rotations based on the resident’s interests.
Faculty Mentors assist residents in developing personalized learning goals and objectives for each of their Individualized Curriculum blocks. We have a structured mentor breakfast in August for the mentors to meet with their resident to review and develop SMART goals for the individualized curriculum blocks in the upcoming academic year. Additionally, residents choose a QI project and scholarly project based on their career goals under the guidance of their mentor and the program director. Residents meet quarterly with the program director to track their individualized curriculum goals. Throughout the year, mentors ensure that their resident is making the adjustment to their duties successfully, assist in the professional and social development of the resident and his/her family as necessary, and serve as an advocate for the resident. In the spring, we have another mentor breakfast for the mentors to meet with the residents and review their progress and plans for the upcoming year.
